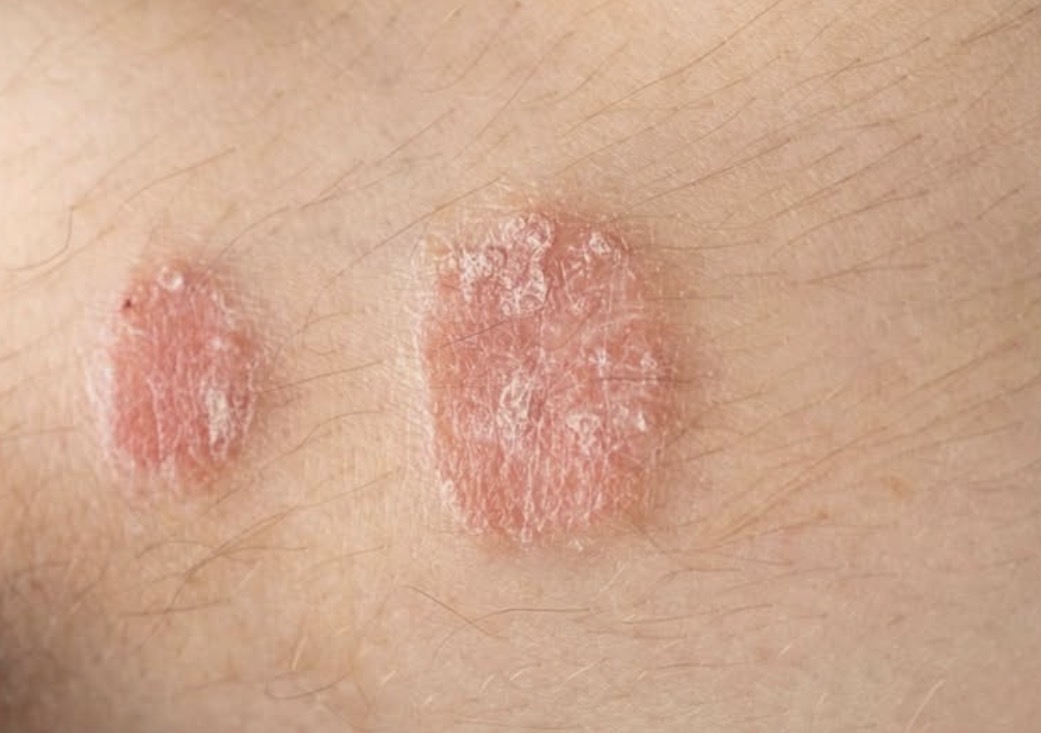
Psoriasis is a chronic autoimmune condition that affects the skin, often leaving those who live with it grappling with both visible discomfort and emotional strain. While many people may assume that psoriasis is merely a cosmetic issue, it is, in fact, a complex interplay of immune system dysfunction, genetic predisposition, and environmental triggers. The immune system in individuals with psoriasis becomes overactive, mistakenly accelerating the life cycle of skin cells. Instead of taking weeks to mature and shed naturally, skin cells can multiply in just days, leading to thick, inflamed patches that can itch, burn, or even crack and bleed. The visibility of these patches can create social and psychological challenges, compounding the physical symptoms. Among the most common and widely recognized forms is plaque psoriasis, which accounts for the majority of cases. Plaque psoriasis manifests as raised, reddish patches covered with silvery scales, most commonly appearing on the scalp, elbows, knees, and sometimes across other regions of the body. These plaques are persistent, often cycling between flare-ups and periods of remission, and their chronic nature necessitates ongoing management. Understanding the nuances of plaque psoriasis—its triggers, symptoms, and progression—is essential for both patients and healthcare providers, as it often sets the standard for diagnosis, treatment approaches, and patient education.
Guttate psoriasis presents a markedly different clinical picture from plaque psoriasis, primarily in its appearance and onset. This variant is characterized by small, pink, drop-shaped lesions scattered over the trunk, arms, and legs. Unlike the thick, raised plaques of plaque psoriasis, guttate lesions are thinner and often appear suddenly, typically following bacterial infections such as streptococcal throat infections. Although guttate psoriasis can resolve on its own, it can also serve as a precursor or trigger for chronic plaque psoriasis in susceptible individuals. Another less common but clinically significant form is pustular psoriasis, which primarily affects adults. It is characterized by inflamed, red skin covered with pus-filled blisters. Pustular psoriasis can appear in localized regions, such as the hands and feet, or it can be generalized, covering larger areas of the body. Although the pustules themselves are sterile and non-infectious, the associated inflammation can be extremely painful. In severe cases, pustular psoriasis may cause systemic symptoms including fever, chills, and fatigue. Proper recognition of these variants is critical because the type of psoriasis determines the treatment plan, informs the expected disease course, and helps predict potential complications. Medical professionals often tailor therapies to address the specific form and severity, aiming to reduce flare-ups and improve patients’ quality of life
Inverse psoriasis, another unique form of the disease, develops in areas of skin folds, such as under the breasts, in the groin, or within the armpits. The lesions in these areas are smooth, shiny, and red, often lacking the silvery scales seen in plaque psoriasis due to the moist environment of the skin folds. Because these areas are prone to friction, sweating, and bacterial overgrowth, irritation and secondary infections can complicate the condition, making management more delicate. Gentle topical therapies, moisture-wicking clothing, and careful hygiene are often recommended to reduce irritation. Erythrodermic psoriasis, on the other hand, is a rare but severe and potentially life-threatening form of the condition. It is characterized by widespread redness, peeling, and scaling across large portions of the body, and it can resemble a severe sunburn. In addition to visible skin symptoms, patients may experience fever, chills, dehydration, and cardiovascular strain. Erythrodermic psoriasis is a medical emergency, requiring immediate hospitalization and intensive management to prevent systemic complications. Both inverse and erythrodermic psoriasis underscore the spectrum of severity within this disease, highlighting the need for prompt recognition, specialized care, and careful monitoring by healthcare professionals.
A pervasive misconception about psoriasis is that it is contagious, which is not the case. Individuals with psoriasis cannot transmit the condition through physical contact, sharing personal items, or casual interaction. The immune-mediated nature of the disease means the problem originates internally, with the body’s own immune system mistakenly triggering rapid skin cell proliferation. Misunderstandings about contagion can exacerbate social stigma, isolation, and psychological distress for patients. Awareness campaigns, patient education, and public information are essential for combating misinformation and fostering empathy and support. Genetics do play a role in susceptibility, so family members may share a predisposition, but the disease does not “spread” in the traditional sense. Environmental factors—stress, infections, injury to the skin (known as the Koebner phenomenon), and certain medications—can trigger flare-ups or exacerbate symptoms in genetically predisposed individuals. Understanding these triggers and educating patients on how to manage or avoid them is a cornerstone of comprehensive psoriasis care.
Treatment for psoriasis depends on the type, severity, and individual patient response. Mild cases often respond well to topical therapies, such as corticosteroid creams, emollients, and coal tar preparations. These treatments aim to reduce inflammation, calm the overactive immune response, and alleviate itching or scaling. Moderate-to-severe cases may require systemic medications, including oral immunomodulators or biologic therapies, which target specific components of the immune system. Biologics have revolutionized the treatment of psoriasis, offering targeted suppression of immune pathways responsible for the rapid turnover of skin cells. Phototherapy, involving controlled exposure to ultraviolet light, is another effective option that can reduce inflammation and slow skin cell proliferation. Beyond direct treatments, lifestyle adjustments are essential to managing flare-ups. Maintaining proper skincare, managing stress, ensuring adequate sleep, eating a balanced diet, avoiding smoking, and moderating alcohol consumption all contribute to reducing the frequency and severity of episodes. A comprehensive approach that combines medical treatment with lifestyle modifications can significantly improve quality of life for individuals with psoriasis.
Finally, it is important to recognize the emotional and psychological dimensions of psoriasis. Visible skin lesions can lead to embarrassment, social anxiety, and even depression, particularly when the disease affects the face, hands, or other prominent areas. Patients may withdraw from social interactions, avoid physical intimacy, or feel stigmatized by the general public. Support networks, counseling, and patient education can help mitigate these effects. Modern approaches to psoriasis management emphasize holistic care that addresses both physical and mental health. Researchers continue to explore new therapies, including advanced biologics, gene-targeted treatments, and immune modulators, offering hope to patients who previously had limited options. Early diagnosis, proper treatment, and continuous medical follow-up are crucial to reducing the physical, emotional, and social burdens of this chronic autoimmune condition. Awareness and education for the general public further enhance understanding, reduce stigma, and encourage compassion for those living with psoriasis. By combining medical, psychological, and lifestyle interventions, individuals with psoriasis can lead fulfilling, empowered lives while effectively managing the complexities of this chronic disease.